 by Dr. Keshava R
by Dr. Keshava R
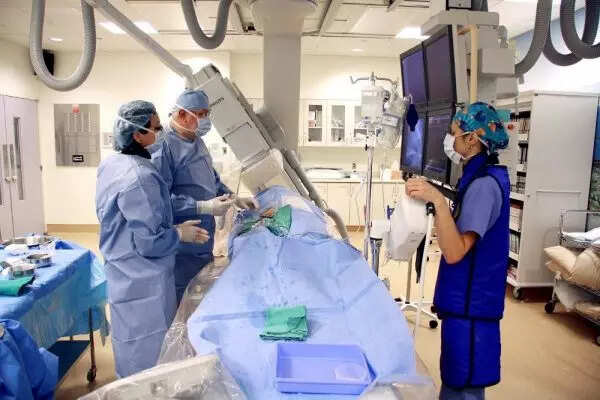
Cardiac catheterization laboratories have evolved from highly specialized research facilities to highly utilized operating rooms where extensive diagnostic testing and interventional treatments are conducted throughout the last half-century, with procedures like Coronary angiography and others being referred to as cardiac catheterization. The room or clinic is equipped with diagnostic imaging technology to check the heart’s arteries and chambers and treat them accordingly.
What is a Cath Lab?
Cardiac catheterization laboratories are specialized hospital rooms where cardiologists detect and treat cardiovascular disease using minimally invasive methods, with a variety of diagnostic and interventional cardiac procedures to treat coronary artery and peripheral vascular disorders.
What is the purpose of these labs?
A quality Cath lab is used to design processes and systems that help optimize patient-team interactions in order to offer high levels of patient safety, with quality being assessed at the level of a single operator, a group, a program, a device, or a system. National registries have been established by cardiovascular societies and organizations to assist institutions in identifying their processes and outcomes in accordance with national standards. To analyse present performance and suggest areas for development, a variety of quality measurement methodologies can be used.
The Cath lab can concentrate on a variety of aspects that affect patient care both directly and indirectly. The competent Cath labs ensure the right quality, with the right patient, and at the right time, and are rewarded for demonstrating high-quality care through collaborative methods that prioritize quality outcomes.
Preventive Measures:
Increased awareness of cardiac emergencies, particularly acute coronary syndromes, including severe bradycardia, through training, is an effective preventive intervention for early heart disease identification. Despite the growth of cardiovascular disorders like coronary artery disease and endemic cardiovascular diseases like RHD in our environment, they still need to be addressed and may benefit from interventional therapies.
Current Statistics available:
Current infection control standards must be followed to limit the occurrence of CIED infections, percutaneous access infections, endocarditis, sepsis, and other infectious problems associated with cardiovascular procedures.
The reported incidence of all linked infections connected with cardiac catheterization was less than 1%, however, the low figures are owing to a lack of event tracking, as infection symptoms normally appear 5-10 days after the procedure. Due to the non-standardization of high-risk evaluation techniques, acceptable complication rates are more difficult to measure in an interventional cardiac laboratory, with many cardiac catheterization studies known to include patients with mild disease (coronary diameter narrowing of less than 50% by visual assessment).
Second, catheterization of the heart’s radial artery might disclose new symptoms necessitating hospitalization. Unless specific clinical information is required, routine right heart catheterization should not be conducted during diagnostic or interventional cardiac catheterization.
The way forward:
New analytical methods are being created to analyze the effectiveness of intervention laboratories, providing crucial data to hospitals that can be utilized to identify areas for improvement.
With the introduction of novel methods for imaging coronary atherosclerosis, non-invasive cardiac imaging has witnessed a rebirth in India, and progress has also been achieved in the field as the evidence base for risk assessment and diagnosis of obstructive coronary artery disease continues to improve.
Dr. Keshava R, Director – Cardiology, Fortis Hospital, Cunningham Road, Bangalore
(DISCLAIMER: The views expressed are solely of the author and ETHealthworld does not necessarily subscribe to it. ETHealthworld.com shall not be responsible for any damage caused to any person / organisation directly or indirectly)